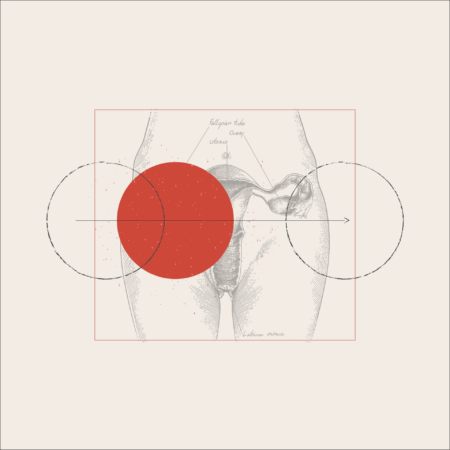
The menstrual cycle is a core component of a woman’s health. Some even go as far as coining it a woman’s fifth vital sign because various aspects, like the length of period flow, the color of blood, and the intensity of bleeding, can confirm if everything is okay—or highlight issues that may be arising inside a woman’s body.
Many focus solely on the period to evaluate the menstrual cycle, however, it is far more complicated. It is also important to know how long the four phases of a woman’s cycle are, confirm if she ovulates, learn how her hormones behave, and determine if she has an elevated hormone baseline.
For decades, women have been striving to meet the standards of an arbitrary “normal” 28-32-day cycle, with a period that lasts for 5 days and ovulation that occurs on cycle day 14. I say it’s arbitrary because our lives have changed drastically since this standard was defined. Looking back even one generation, most will notice that their parents conceived their first child at a significantly younger age than women today. More women are striving to acquire higher education, hit career milestones, travel, find the right partner, and enjoy life together before growing their families. Unfortunately, while doing all these things, our bodies are aging and it becomes harder to conceive naturally.
It is critical to learn each woman’s unique hormone profile, detect fluctuations, then determine what is happening in her cycle.
So what happens if you do not have a 28-32-day cycle? What happens if you don’t have a regular period? Do you still ovulate? Can you still get pregnant naturally? These are questions that flood the minds of women who do not fit the mold of that “normal” cycle. These women make up over 35 percent of the female population, including those with irregular periods, imbalanced hormones, or reproductive disorders such as polycystic ovary syndrome (PCOS) or endometriosis.
If a woman has reproductive disorders, her hormone profile will be very different from someone who does not. For example, in order for ovulation to happen, the luteinizing hormone (or LH levels) must elevate to signal the ovary to release the egg. However, how is that spike detected? Does it have to reach some predetermined threshold? If so, what happens if a woman has systemic elevated LH levels because she has PCOS? She’s not always ovulating. This is why personalized healthcare is so important. It is critical to learn each woman’s unique hormone profile, detect fluctuations, then determine what is happening in her cycle. Without this information, medical advice and care is being based on standards that are irrelevant for individual woman.

With the advancement of technology (and a daily blood draw at a fertility clinic), it has become a lot more accessible to get the personalized data we need to truly understand each woman’s unique fertility profile. This enabled clinicians to capture and monitor daily hormone levels throughout a cycle, but at the height of the COVID-19 pandemic, fertility clinics were being asked to close their doors because fertility care was considered an elective procedure. Couples and clinics were left in a horrible state of limbo where they weren’t sure how to proceed.
This gave our technology at Oova an amazing opportunity to shine. We created a urine test to monitor quantitative levels of fertility hormones in the privacy of a woman’s home with the same accuracy as a blood test. The only link missing was for a clinician to be able to view this data seamlessly. We solved this problem by creating a HIPAA compliant dashboard: when a woman gets her hormone results in the Oova app, her clinician sees them in their dashboard, all in real-time. This has become a true game changer for the healthcare industry. As healthcare rapidly expands beyond the hospital—with COVID-19 fueling an even greater demand for at-home monitoring—patients no longer want to get poked and prodded unnecessarily. Patients also don’t want to go to the clinic for routine work that can be done in their home. Now clinics can continue to monitor their patients remotely, saving them time, money and resources, while patients are testing in the privacy of their homes.
But it is not enough to just monitor hormone levels. The critical element is learning and embracing every woman’s unique hormone profile. This is vital for women who have irregular cycles or reproductive disorders. These women may have trends, baselines, and hormone behavior that is completely consistent for them each cycle, but off from the “normal” curve. By learning every woman’s unique fertility profile, we can determine if her curve is normal for her body.
Let Oova decode your fertility by ordering your kit today
The past year has been an unprecedented time for society. Every industry was challenged and put to the test. However, no industry was challenged as heavily as the healthcare system, from patient care, clinician demand, medical access, to what is considered an elective procedure. It highlighted how flawed our system was and how desperately change was needed. We can start addressing this change by applying technology to enable personalized care, and getting to the root of health issues.
Oova is on a mission to revolutionize healthcare and we started with an area that was in dire need of innovation. There has been such little innovation, especially when it comes to fertility, as most at-home urine testing (think regular ovulation predictor kits) has been limited to a binary positive or negative results. With the incorporation of technological advancements, we can now get accurate quantitative values for critical biomarkers, providing clinical data in the privacy of your home. This is not only easing the health journey for women but also increasing accessibility for fertility care for those who cannot afford to go to the clinic every day. We have just unveiled the tip of the iceberg when it comes to what our technology can do. We plan to disrupt as many areas of healthcare that we can. This is just the beginning of Oova’s journey.
Dr. Amy Divaraniya, a PhD in Biomedical Sciences with a focus on Genetics and Genomics from Mount Sinai School of Medicine, is the founder and CEO of Oova. While trying to conceive for 18 months, Amy was shocked by the lack of precise, science-based fertility options. This drove her to develop Oova’s lab-grade fertility translator to track multiple hormones and create a personalized fertility profile to indicate specific moments in a woman’s cycle.